
What is type 1 diabetes?
Type 1 diabetes affects the body’s ability to convert sugar from food into energy. Click here to learn more about the symptoms of type 1 diabetes and how to manage after a diagnosis.
Are you exploring ways to manage type 1 diabetes during pregnancy? If you have type 1 diabetes and are planning to become pregnant or are pregnant already, you can have a completely healthy pregnancy and baby. The chance of your baby developing type 1 diabetes, if you have type 1 diabetes, is only 5%1. However, it is still important to consider your risks and keep your diabetes under control during pregnancy to reduce risks to you and your baby.
If you have either type 1 or type 2 diabetes, it is very important to plan a pregnancy to keep you and your baby healthy. If your blood glucose is high at the time you become pregnant, and during the first 6-8 weeks, it can be harmful to your baby. The risks to you can include hypoglycaemia (hypo), poor hypo awareness (you don’t realise when your blood glucose is low), miscarriage and having a very large baby (which can cause problems during labour)
Checklist to planning a healthy pregnancy
Pre-Pregnancy Care
Gestational diabetes is a form of diabetes (raised level of glucose in the blood) that is diagnosed during pregnancy. In most cases there will be no symptoms. A pregnancy complicated by gestational diabetes is considered high risk and will require specialised care.
The insulin hormone may change during pregnancy. In addition, your body may not make as much insulin as it requires during pregnancy. Either of these issues can result in high blood glucose levels. If left untreated, high blood glucose levels may cause health problems for you and your baby.
Risk factors
Gestational diabetes is usually diagnosed with an oral glucose tolerant test (GTT). The following are risk factors that indicate a glucose tolerance test is necessary:
Treatment & Monitoring
Each patient’s treatment plan will be individual and decided on by yourself and your specialist team. It will be necessary to monitor your blood glucose levels for the duration of your pregnancy. The standard treatment for gestational diabetes is diet and lifestyle changes, but many women also require medication such as insulin injections and/or tablets. If you do require treatment, it is generally only for the duration of your pregnancy.
Follow up
There is a high risk of gestational diabetes returning in a future pregnancy. There is also a high chance of developing type 2 diabetes in the future. Research shows that maintaining a healthy weight, keeping a healthy diet and taking regular exercise, may prevent or delay the development of type 2 diabetes.
Having gestational diabetes should not prevent you from breastfeeding your baby. Breast milk following gestational diabetes will be the same as the breastmilk of a woman who has not had gestational diabetes. For advice and support on breastfeeding please contact your local breastfeeding team.
It is recommended that you have a diabetes test at around 6 weeks after you give birth. It is also recommended you have an annual diabetes screening and you consider attending a diabetes prevention programme.
It is advised that if you are planning another pregnancy, you make sure that your diabetes screening is up-to-date, and your blood glucose is within normal limits. If not planning another pregnancy, please discuss a reliable method of contraception with your Healthcare Practitioners. If you find yourself unexpectedly pregnant you should seek medical advice immediately.
Managing type 1 diabetes and pregnancy can be a challenge. Type 1 diabetes pregnancy risks include:
To lower these type 1 diabetes pregnancy risks and help you and your little one experience pregnancy as safely as possible5:
Read on to find out more on how to plan a pregnancy when you have type 1 diabetes.
How can you manage type 1 diabetes and pregnancy? If you have type 1 diabetes and are planning on getting pregnant, here are a few steps to prepare for a healthy pregnancy and reduce type 1 diabetes pregnancy risks:
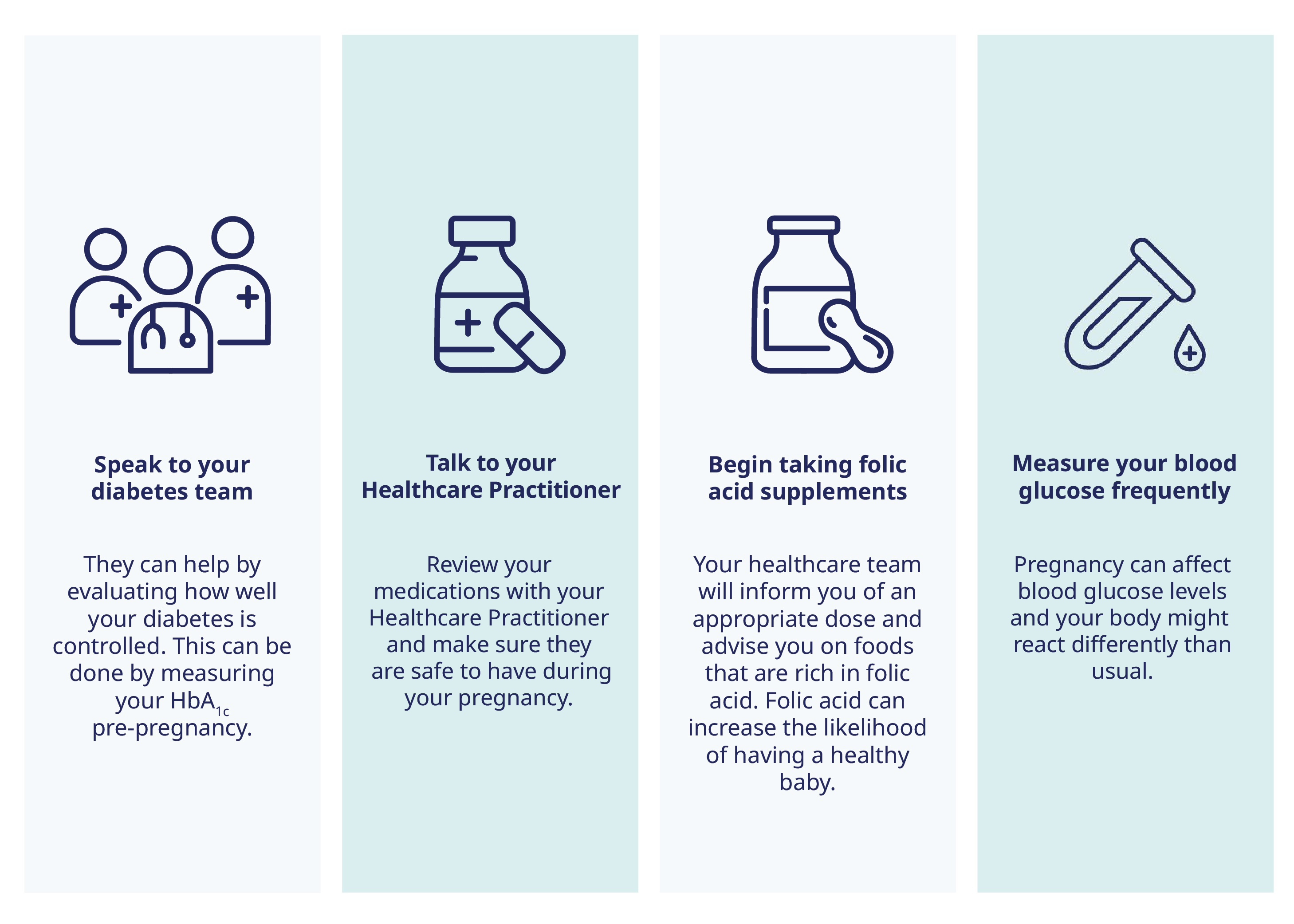
Top tip: If your pregnancy was unplanned, get in touch with your doctor and healthcare team as soon as possible; they can advise you on how to best manage your type 1 diabetes during pregnancy7.
It is vital to contact your healthcare team to adjust your diabetes management plan as soon as you discover you are pregnant. Your doctor may recommend changes to your current diabetes treatment, for example, you may be advised to adjust your insulin doses8. During pregnancy, it is even more important that you regularly monitor your blood blood glucose levels, adhere to frequent check-ups with your medical team and follow a healthy and balanced diet1,9.
Top tip: It’s essential for you to avoid alcohol and smoking to maintain a healthy pregnancy9.
You can expect a full-term pregnancy and a natural birth, although you may be advised to induce labour or have a caesarean section for you and your baby’s protection1.
During your delivery, your blood glucose will be under constant monitoring. Your doctor may formulate an ‘insulin plan’, which includes steps to monitor and regulate your blood levels during and after your delivery if needed, and the area of your body where insulin should be injected8,10.
Both your and the baby’s blood glucose levels will be closely monitored after delivery. This is likely to include a heel-prick blood test for your baby8. If your baby’s blood glucose is low, they may need extra support, such as a drip or feeding tube, which will be provided by Healthcare Practitioners within your Healthcare team11. As breast milk contains lactose, a type of sugar, every time you breastfeed, your glucose levels can drop. If you are breastfeeding, your Healthcare Practitioner may adjust your insulin dosing and advise you to have a meal or light snack before each feed12.
It is important to continue looking after yourself and stay healthy after you have given birth. Try to maintain a healthy lifestyle by being active, eating a balanced diet, monitoring your blood glucose levels, and reaching out for support to your family, friends and healthcare team whenever needed.
Type 1 diabetes and pregnancy can seem stressful and overwhelming. But with careful planning and paying attention to your medical needs, you are likely to have a completely healthy pregnancy1,5.
February 2024. IE23DI00248


